The numbers keep rising. We are inundated with data about the modeling of cases, when the apex will hit and how to flatten the curve. New York City is the epicenter of the outbreak with 72,000 people testing positive and the death rate climbing to 2,500. We are all at risk.
I guess I can be considered one of the lucky (recovered) statistics, but two weeks out from my traumatic hospitalization, I am still left with the feeling, “this is no joke.”
We had returned from a planned family vacation in the Caribbean on Sunday, March 8 when the warning signs were just beginning to be noticed. The airports were still filled with travelers, and we were being admonished to cover our coughs and wash our hands regularly. I began to feel signs of fatigue that week – a slight cough, some nausea and what we now know as the telltale sign of reduced appetite and lack of taste. I went about my business and was probably in a state of denial that something could be seriously wrong.
Yes, my age (68) put me in a high-risk category but my underlying health was excellent. I continued my regular four-day-a-week exercise routine, alternating between my mile swim one day and the aerobic joy of the elliptical and weight machines.
A week later, however, the signs that something was not right began to creep up on me. Walks in Central Park were not easy. I began to feel out of breath quickly. My wife, Susan, would continue to walk while I sat down on the nearest bench.
It was becoming clear that the incidence of COVID-19 cases had taken a turn upward in the city. However, it was not easy to overcome my stubbornness and insistence of others that it was time to call the doctor. I left a message and he called me back the next day. He prescribed a strong dose of azithromycin and an albuterol inhaler for my shortness of breath.
Confusion Around Testing
None of this seemed to work. I had no fever, though, and the conventional wisdom that week of the rapidly spreading virus was that a fever was the telltale sign. There was much confusion around testing so I doubted I would be eligible. I could just ride it out despite the waves of nausea and loss of appetite I was experiencing.
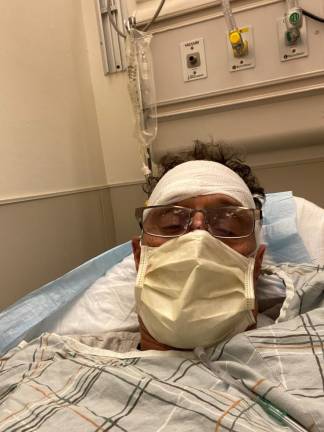
I woke up Sunday morning, March 22, merely a week after I began feeling ill, and headed to the kitchen as is my normal early morning habit. Susan had meandered into the living room. I got up from my chair and was about to pour myself my morning orange juice when the room began to spin. The next thing I knew I was lying in a pool of blood on the kitchen floor, having gashed my face on the counter on my way down.
Fainting is scary. Susan rushed in and had the presence of mind to call 911. She implored the EMS worker not to take me to the hospital since the virus cases there were on the rise. The paramedic was having none of it: “Get his shoes and socks on, take his coat and tell me what hospital you want to be taken to.” In retrospect, both of us were grateful for her no-nonsense approach. It is true that those first responders are heroes.
Susan was not allowed to accompany me in the ambulance. I saw her wave to me through the rear window, a tear in her eye, wondering if I would be OK. No family members are allowed in the age of the virus.
The Mount Sinai emergency room that Sunday morning was not crowded. I was attended to relatively quickly by nurses and doctors garbed in their PPEs. I was more concerned by my aching gashed head than by anything else.
One of the ER doctors noticed that my blood oxygen level was low and that there was some abnormality in in my lungs. They swabbed my nose and tested me for COVID-19. It was now standard procedure for someone with my symptoms. Hours later, the test came back. I was positive. I was put on oxygen and told I would have to be hospitalized. I had what they diagnosed as COVID-induced pneumonia.
By a stroke of luck — my passing out, smashing my head and ending up the ER, I was now in a safe space and being taken care of. Would I just have continued to suffer at home and never be tested without the accident? The vicissitudes of the virus make this somewhat of a crapshoot.
On Lockdown
I spent two nights in the hospital. They had converted the orthopedic floor to a COVID-19 wing. The nurse said the other day they had two patients – now they had twenty and were anticipating many more. I was placed in a room with another COVID-19 positive patient. He was in much worse shape than I was. He had an oxygen mask, spent the entire night wheezing and coughing and could barely speak. The next day he was taken to the ICU and put on a ventilator. I think to this day, “Did he make it?”
There was a surreal feel to the hospital. The staff would come in and out, incessantly changing their masks and disposable gowns. You were not allowed to leave your room and peak out in the hallway. You were on lockdown. Bless the souls of those workers who were kind, caring and doing the best they could in an ever-changing environment of new protocols and tough decisions. You could tell they were struggling as well, yet doing the best they could.
The second night in the hospital, I was off the oxygen and my vital numbers were good enough for them to send me home the next day. I was a moderate case and the hospital needed the space for the more serious cases to come. The hospital attendant wheeled me out to the street, gave me two masks and gloves, hailed a taxi on Fifth Avenue and I was at my West Side home in a few minutes. No one picks you up at the hospital in the era of the coronavirus. I didn’t share a word with the taxi driver – gave him a twenty-dollar bill and thanked him. The entire experience was eerie.
Susan and I spent the next seven days in self-isolation, never crossing paths in our apartment. She had some symptoms as well and had been told by the ER doctor that she that she was likely positive, too. She was never tested but we are now fully recovered and staying home like everyone else. From what I understand, I am now not contagious and probably have some level of immunity. I consider myself lucky. I was taken care of “under the wire.” The virus has spread like wildfire over the last two weeks with the medical resources being stretched beyond capacity. I’m not sure others will be so fortunate.
Stephan Russo is a West Side Spirit contributor, and an Upper West Side resident since 1975. He served as the Executive Director of Goddard Riverside Community Center from 1998-2017.
“Get his shoes and socks on, take his coat and tell me what hospital you want to be taken to,” said the paramedic.